 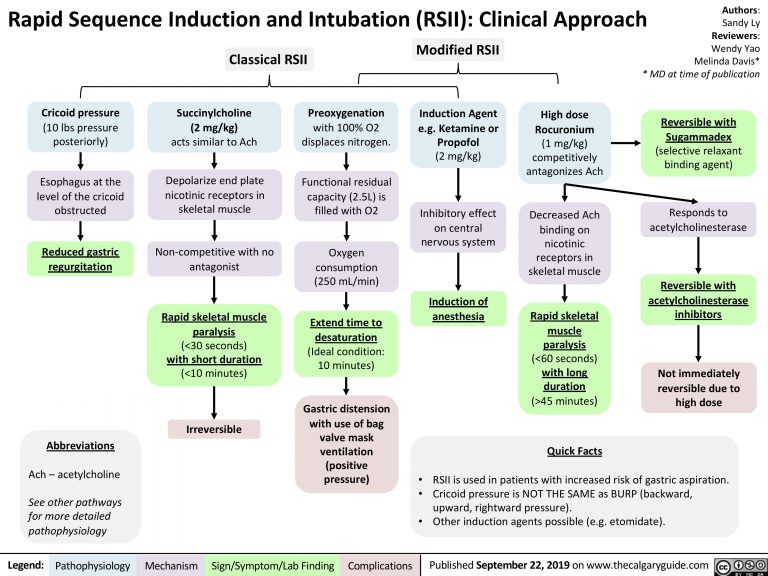
The anesthesiologists have the options of using gas agents for induction. In the operating room, we have - it's a much more controlled environment, we have more time. When we talk about RSI in the emergency department, that's rapid sequence intubation, that's pretty rapid compared to what we do in the operating room. 
So an induction agent is given to sedate the patient appropriately so that they can then receive the paralytic that allows the patient to be intubated safely and quickly. I'll start and we'll consider what's going to be our induction agent. So once we've decided that we're going to intubate the patient - we've made our plan, we're starting to get our supplies ready, you know, they're getting the laryngoscope, we have RT at the bedside as well. Part of my job, as well as providing the medications for the initial intubation itself is making sure we have the appropriate analgesic plan, and then the postintubation sedation as well so that we can keep these patients comfortable while we continue with our treatments including imaging and any therapeutics they may need. If we have any inkling - we won't have labs back usually on a trauma patient - but do we have any reason to suspect this patient may have liver or renal dysfunction? And that will help us decide which medications we choose to use. We're going to look at the patient's size. We'll talk about the contraindications we have for certain medications. So first things first, we want to assess the patients themselves, look for any obvious contraindications. Once the team has made the decision that they're going to intubate the patient, whether it's due to the patient's injuries themselves for pain control, or due to altered mental status, I come in and I have my fantastic RSI kit ready to go. So I'll also talk to you guys a little bit today about RSI medications as part of our airway management for our trauma patients. I've been here for about two years, and I've been part of the team for all of our critical patients who come into the emergency department, including but not limited to our trauma patients. 
I am a clinical pharmacist here in the emergency department at the University of Chicago Medical Center. The authors concluded that when used for RSI, although patients administered ketamine showed greater haemodynamic instability, this had no important impact on either the first-pass success rate or other relevant clinical outcomes.Hello, my name is Laura Celmins. Similarly, there were no differences in other clinical outcomes explored including final mortality (p = 0.348), length of intensive care unit stay (p = 0.99), ventilator days (p = 0.735) and overall hospital stay (p = 0.32). The ketamine patients had a significantly faster initial heart rate (105.0 vs 97.7, p = 0.003) and were more hypotensive (114.2 vs 139.3 mmHg, p 0.999). 
No impact on clinical outcomesĪ total of 620 patients, of whom 19.9% received ketamine, were included in the retrospective analysis. For example, single dose use of etomidate may increase 28-day mortality, whereas ketamine use could increase the risk of cardiac arrest. Nevertheless, both are associated with potential adverse effects which could affect clinical outcomes. Despite being a standard procedure, a recent survey identified significant variation in practice, prompting called for international RSI guidelines.īoth ketamine and etomidate are commonly used sedatives for RSI during emergency tracheal intubation. Ideally, the RSI procedure should allow for rapid and optimal intubation conditions through increasing the first-pass intubation rate whilst reducing adverse events in severely injured patients. RSI represents the set of actions undertaken during induction of anaesthesia that secures the airway in trauma patients at risk of aspiration or regurgitation of gastric contents, to enable emergency orotracheal intubation. Patients given ketamine were propensity-matched 1:3 with etomidate and the results adjusted for injury severity and confounding baseline characteristics. The team retrospectively compared both sedatives, not only in terms of the effect on the first-pass success rate but also with respect to clinical outcomes. Published in the journal BMC Emergency Medicine, Korean researchers considered whether the potential adverse effects of ketamine and etomidate could affect the first-pass success rate during rapid sequence intubation (RSI) in trauma patients. Although ketamine use increases haemodynamic instability during rapid sequence intubation in trauma patients, it does not significantly affect the first-pass success rate compared to etomidate, according to a retrospective analysis. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
